Shoulder Pain While Throwing?
Shoulder pain after and during pitching is common in baseball, as well as other overhead throwing sports. Common diagnosis are: rotator cuff tendonitis, labral tear, bicipital tendonitis, subacromial impingement, and bursitis. It is treatable and recovery is possible within weeks to months with the correct treatment plan. Return to throwing is possible.
Allow me to walk you through some of the current information about how to avoid shoulder surgery.
I’ve played and still play baseball. Many of my teammates over the years have had a rotator cuff and/ or labral repairs and never regained their ability to throw with confidence again.
Since I play on an adult league team now, many of these guys are 10+ years post op. Most of them never strengthened their shoulder before the surgery and lagged on the rehab afterward… which is why many adult league hardball players fight over first/ second base and beg to only be on the hill for a few innings a week.
I’ve done all the research you’ll need in this article.
You won’t need to go anywhere else!
In fact, I’m in the process of creating a free rehab shoulder course for throwers for you as well. It will be linked here where it’s ready.
Enjoy the article.
By the way, if you’re experiencing any neck tightness or midback/ shoulder blade tightness, pain or aches then you should be reading this other article I wrote.
Your shoulder pain is more than likely related to a neck issue. I’ll be clear, if you treat this type of shoulder pain as a “shoulder condition,” not symptoms referred from your neck/ nerve, then you’ll be in pain for a very long time. You will be very frustrated.
Please the other article for more info to see if you fit that description.
Dr. Sebastian Gonzales DC, DACBSP®, CSCS
EXPECTATIONS WHEN YOU
COME SEE US IN COSTA MESA:
MORE THAN 50% IMPROVEMENT WITHIN 4-6 SESSIONS
Most Cases
MORE RELIEF WITH LESS RISK
We Only Use High Reward/Low Risk Treatments
NO RIDICULOUS LONG-TERM TREATMENT PLANS
MORE ATTENTION WITH A SKILLED GUIDE
Even Though our Costa Mesa Chiropractor are Not A "Real Doctor" 🙂
MORE THAN A TYPICAL COSTA MESA CHIROPRACTOR
No Bone Cracking Required To Feel Good
NO QUACKERY
Dr. Gonzales & Costantino Only Uses Current Evidence-Informed Methods
CLICK HERE TO BOOK YOUR APPOINTMENT WITH A COSTA MESA CHIROPRACTOR
Avoid Rotator Cuff Surgery
9 facts about Shoulder Rotator Cuff tears that all pitchers shoulder know, and so much more
When pitchers become more advanced in their play and position, rotator cuff tears of the shoulder can often become surgical cases.
This article will educate pitchers and players on how they can avoid surgery and the potential loss of their baseball and pitching careers.
Why do you need to know 30+ pages about rotator cuff tears?
As a pitcher, hearing that you could potentially have a rotator cuff tear is probably one of the worst things you could hear. Not only can rotator cuff tears be very painful, but they can also often be detrimental to careers.
So, can they be prevented?
Yes! Scientific research has indicated that most rotators cuff tears are atraumatic, or in other words, they are “build-up/ overuse” conditions.
The goal of this article is to assist you in developing an awareness of how these tears tend to develop in pitchers and to assist you in learning what steps need to be taken in order to prevent these tears.
If you’re like most people, you came here for exercises. If this is you, then skip to the Shoulder/ Shoulder Blade Video Mini-Guide. I didn’t create the full course yet, but I thought releasing a mini-guide would be perfect for the motivated athletes who can’t wait for me.
I gave it the name An Introduction Into The 9 Best Corrective Exercises For SICK Scapula because the shoulder blade is the key to preventing and rehabbing many rotator cuff issues.
The exercises are simple to perform, especially if pain is minimal. When the shoulder becomes a “hot case” then it becomes more complicated because pain corrupts movement.
Get it now and if you don’t like it then just email me for a refund. Simple.
These days, a more common and more “exotic” injury to have is an ulnar collateral ligament (UCL) tear. This type of tear often leads to Tommy John surgery, which replaces the elbow ligament after a tear.
While the “Tommy John” procedure is becoming increasingly more common, the procedure actually yields a much higher percentage of players returning to play when compared to procedures meant to correct a rotator cuff tear or shoulder labral tear.
As of 2014, rotator cuff tears in the MLB seem to be on the decline, whereas UCL injuries seem to be on the rise.
In 1997, both types of injuries occurred at 25 incidents per season.
In 2003, rotator cuff tears continued to occur in the mid 20’s per season, while UCL occurrences jumped to nearly 60 players per season.
As of 2014, rotator cuff tears have now dropped to 14 incidents per season and UCL injuries remain high, in the 60’s.(1)

Is this showing a tread on rotator cuff injuries fading off into the sunset?
No, not at all.
Both shoulder and elbow injuries come from a break down of the lower body, trunk and shoulder blade region from a strength, stabilization or pitching form fault.
Rotator cuff tears are extremely common and can occur in any of the 4 cuff muscles:
• Supraspinatus
• Infraspinatus
• Teres minor
• Subscapularis
Rotator cuff tears can also be asymptomatic.
In fact, it has been estimated that 66% of cuff tears do not present with pain.
Of the 33% of cases that actually do present with pain, typically only 20% of those cases actually seek medical attention for the condition. (16) Tears will typically respond to conservative forms of treatment, but the pain can often return after the rehabilitation process is “complete.”
The pain typically returns when the tear is subjected to expansion.
What is expansion?
Expansion is where a previously sustained tear becomes larger, or when “tendonitis” turns in to a tear.
You read that right: tears can get larger over time.
One major thing you can take away from the research is that there is no such thing as “completion” of rehabilitation. Rehab is an on-going process. This does not mean, however, that the pitcher needs to be present in a healthcare facility multiple times a week.
Let’s get another thing straight…
Just because a majority of rotator cuff tears do not cause pain, this does not mean that they are not eventually going to.
Once a pitcher has sustained a rotator cuff tear, he or she will always have a rotator cuff tear.
This does not mean that all activity needs to immediately stop and he or she should get themselves in to an operating room as soon as possible.
Rehabilitation is a weekly process and, in many cases, will end up being a part of your daily warm-up or cool down. This should always be the mental approach to rehab on any injury.
We will go in to further details on some of the things that can be done for rehab later in this article.
Why is it so much more complicated to surgically repair a rotator cuff?
To start, the structure that is being repaired is much more rigid.
Ligaments are very firm, while muscles and tendons are very pliable. This pliability is required for after a repair.
It is the dynamic nature of the muscles and tendons of the rotator cuff that could lead to a re-tear.
Second is the nature of the joint that being repaired.
When you compare the elbow to the shoulder, the elbow is very simple and stable. The shoulder joint is a ball and socket joint. By nature, ball and socket joints yield large amounts of motion and instability. Baseball pitchers just so happen to be the poster boys for shoulder instability and laxity.
When a joint becomes laxer, the surrounding muscles and tendons take on the extra task of stabilizing that joint through its large range of motion.
Third is the typical loss in range of motion, due to stiffness, after the surgical repair.
A loss (or gain for that matter) of range of motion, in a pitcher, for any reason, can be a detrimental event. The amount of range of motion that you lose, post-op, is reason enough to seek and attempt non-surgical rehabilitation, if at all possible.
Below, I have compiled a short list of pitchers who have sustained rotator cuff tears in just the past few years. Keep in mind that this list includes pitchers with reported “tendonitis” and “inflammation,” since both of these conditions also fall under the section of diagnostic imaging called “interstitial tears.” The term “interstitial” refers to a small tear within the fibers of the structure and it does not extend through to the ends of said structure.
• Pedro Martinez
• Joey Eischen
• Kris Benson
• Cliff Politte
• Mark Mulder
• Matt Clement
• Bartolo Colon
• Ryan Wagner
• Freddy Garcia
• Tom Gordon
• Johan Santana
• Brandon Webb
• Kerry Wood
• Don Drysdale
• Ben McDonald
• John Rocker
• Wayne Simpson
• Mike Scott
• Matt Keough
• Mark Fidrych
• Steve Busby
• Don Gullett
So, what can cause a rotator cuff tear in pitchers?
• Poor pitching mechanics
• Weakness in the rotator cuff/shoulder blade
• Haphazard throwing calendar
• Weakness in the lower body and core
If you would like a recap of anatomy and physiology, click through to bottom of page:
Shoulder Pain Facts #1-3
Fact #1:
13%: The percentage of the force generated by the shoulder when pitching. (9,10,11,26)
Notice that this is not a large percentage at all. This means that much your velocity in pitching will does not come from the arm/shoulder.
So then where does it come from? See the fact below to find out.
Fact #2:
51-55%: The percentage of force generated by the trunk, pelvis, and legs when pitching. (9,10,11,26)
This percentage is huge!
The power that your lower body produces is where most of your pitching velocity comes from. Great pitchers don’t just glide off the mound, they drive off the mound.
By using your lower body more during pitches, you could just end up saving your shoulder and elbow from a lot of pain and frustration later on.
Fact #3:
2 million: The number of rotator cuff cases reported every year!
This number is changing every year, I’m sure, but the take away point here is not so much the exact number, as it is the raw volume!
Rotator cuff tears are, unfortunately, very common. The good news, though, is that they are very preventable with the right rehab/exercise program in place.
The right kind of program should only take you an extra 15-20 minutes a day and it only needs to be done a few days of the week, assuming that you are already doing regular workouts for pitching.
If you would like a glimpse at a program we do have a free intro course available.
Shoulder Pain Facts #4-6
Fact #4:
33%: The percentage of tears requiring surgery.(16)
This number represents only advanced tears. Most of the time, pitchers will present with a lot of warning signs years before actually suffering a tear of this magnitude.
Fact #5:
$21,800: The average cost of a rotator cuff surgery.
Obviously, this number can vary greatly based upon hospital costs, surgeon fees, anesthesiologist fees and much more. It can also range based upon the location where the procedure takes place and the skill levels of the doctors involved.(12)
Fact #6:
3: The average number of seasons it takes for a pitcher to degrade after a surgery.
The most common predictor of future injury is past injury. Once a tear has occurred, rehab needs to be done all year-round. There is no off-season for rehab on a rotator cuff tear. “Fear avoidance” is also a huge hurdle to get through while rehabbing and returning to play.
Fear avoidance is when athletes allow themselves to perform below their potential for fear of reinjuring themselves. They avoid performing up to their potential, even when their maximum potential is still safe. In pitchers, they might fear that throwing harder will cause them to hurt their shoulder again. If not addressed, the decrease in performance will definitely show, and may also become the new norm for that player.
Shoulder Pain Facts #7-9
Fact #7:
8%: The percentage of pitchers with full thickness tears who will ever pitch again. (25,30)
Wow, 8% ever throw again… this stat scared me when I saw it.
In fact, this was one of my major reasons for creating an article of this length and detail. You need to know!
Fact #8:
1: The number of seasons lost, minimum, if surgery is performed.
The time it takes to recover from a rotator cuff surgery can vary, but typically speaking, it can take months.
If you are in-season when the tear happens, that is the end of your season. The healing time for the rotator cuff, by itself, will take months. When you add in the time it will take to get back in to pitching shape, you are now on an entirely different timeline.
Hopefully, during your healing time, you will be able to work with your strength and conditioning coach on shoulder strength. Once it is fully healed, the legs, hips, and back are now waiting to be conditioned.
Fact #9:
12: The number of weeks of physiotherapy found to rival subacromial decompression surgery in success rate. 13
That’s right! In some cases, hard work was just as effective as surgery! Both treatments showed that a majority of the improvement made in the athlete, was made within the first three months.
So how do you know if you should pursue surgery or physiotherapy?
A majority of doctors will agree that if you have not seen any improvement in the shoulder within six months of performing less invasive procedures (physiotherapy), then decompression surgery will likely be a better option.
Rehab methods can include: (8)
- Passive and active range of motion exercises
- Selective capsular stretching
- Core strengthening and stabilization
- Neuromuscular exercise
- Strengthening of the rotator cuff, deltoid, and periscapular musculature
Anatomy of the Shoulder
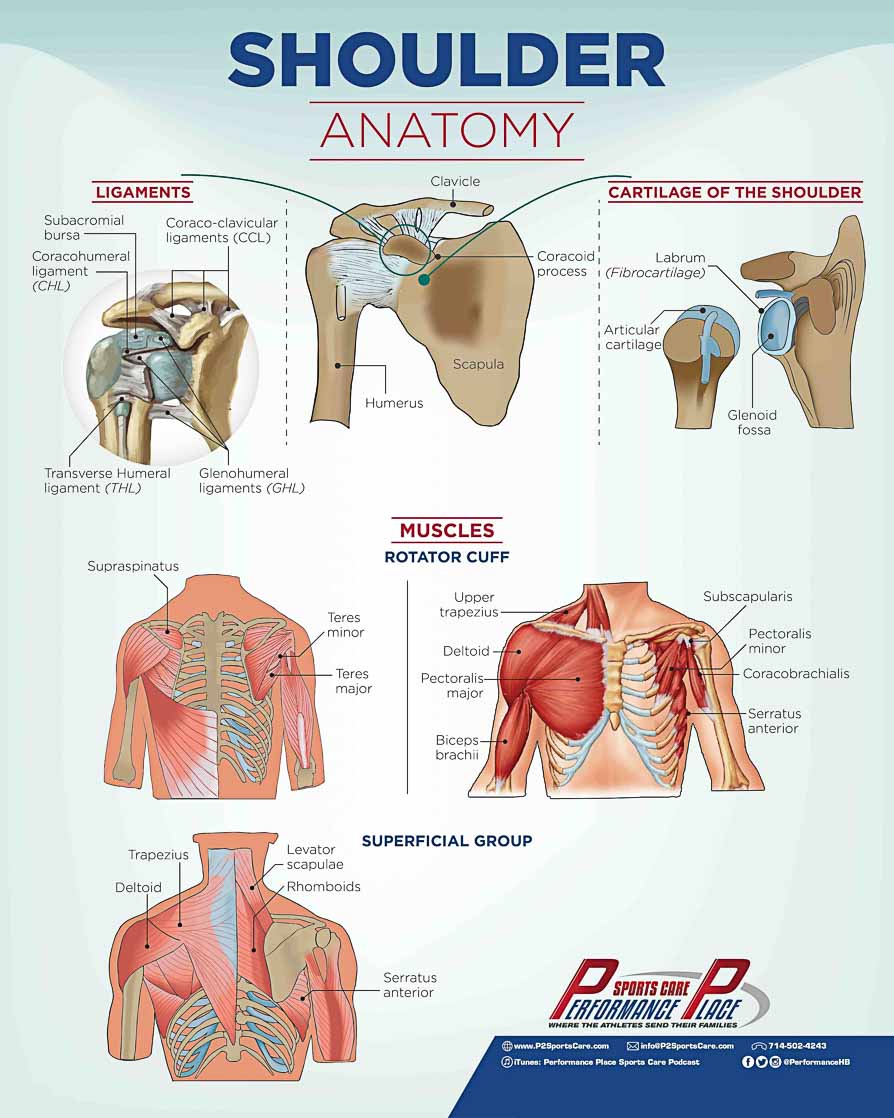
To really understand the different types of rotator cuff tears we have to start with and understanding of the shoulder, shoulder blade, and trunk. The shoulder, or glenohumeral joint, is considered a ball and socket joint.
The ball of the joint is the humeral head, or the top portion of the arm bone, and the socket is made by the shoulder blade, or the scapula.
Share this Image On Your Site
NOTE: IF YOU ARE USING A DIVI WORDPRESS THEME YOU MUST EMBED IN THE CODE MODULE… NOT THE TEXT MODULE
Important anatomical structures surrounding the joint include bones, ligaments, cartilage, muscles, and tendons.
Bones of the Shoulder
The bones creating the shoulder joint proper are:
• the humerus
• the scapula
The shoulder joint is held to the body by one bony attachment from the front side of the body.
The following bones make up that bony attachment:
• the clavicle
• the sternum
It is extremely important to remember that the shoulder has only one bony attachment site that keeps it on the rest of the body. Especially when considering methods of rehabilitation, and the overall health of the shoulder, the rotator cuff, the labrum, and the shoulder blade.
Why is this important to remember?
Because, a single bony attachment is not intended to take on the load of an entire limb!
If the arm and shoulder are being used properly, then the weight and the work load should be spread out throughout the area.
Think of it this way…
When someone fall off of their bike of if they fall out of a tree, where do they usually injure themselves? More often than not, they will suffer a broken collarbone of a sprain in the AC (acromioclavicular) joint.
The shoulder and rotator cuff will only function well if the load is spread to the shoulder blade. Muscles of the shoulder blade play a critical role in saving the rotator cuff.
To put it simply, in order to save the rotator cuff, the shoulder blade AND torso need to be strong and functional.
Cartilages of the Shoulder
As for cartilages, there are two important types in the shoulder joint.
• Articular Cartilage
• Fibrocartilage
The articular cartilage is located on the “ball” of the humeral head and the face of the “socket,” otherwise known as the glenoid fossa.
The purpose of the articular cartilage is to decrease friction in the joint and to create a smooth surface for two bones to slide against each other.
Fibrocartilage is made of a very different substance than articular cartilage and is therefore used for a very different purpose. In the shoulder, fibrocartilage is located on the face of the glenoid fossa, or socket.
The labrum of the shoulder is located there and is made of fibrocartilage.
The labrum is much like an O-ring. It creates a tight seal meant to provide extra stabilization of this very mobile joint.
70% of shoulder-joint stability relies on this cartilage being intact. It is no wonder why labral tears have such a profound effect on shoulder stability.
Ligaments of the Shoulder
Ligaments of the shoulder come from many places and they surround the shoulder.
Here are some of the noteworthy ligaments of the shoulder:
• Glenohumeral Ligaments (GHL)
• Coraco-acromial Ligament (CAL)
• Coraco-clavicular Ligaments (CCL)
• Transverse Humeral Ligament (THL)
The Glenohumeral Ligaments:
These ligaments create the most stabilization for the glenohumeral joint and prevent the shoulder from dislocating.
The glenohumeral ligaments are: the superior glenohumeral ligament, the middle glenohumeral ligament, and the inferior glenohumeral ligament.
The Coraco-acromial Ligament:
The Coraco-acromial Ligament, which is commonly thickened in causes of shoulder impingement syndrome. Impingement syndrome is commonly found in cases of rotator cuff tears in pitchers.
The Coraco-clavicular Ligament:
The Coraco-clavicular Ligament is composed of two ligaments: the trapezoid ligament and conoid ligament.
These two ligaments connect the coracoid process of the scapula to the clavicle.
The Coraco-clavicular Ligament is extremely strong and keeps the shoulder attached to the rest of the body in that single bony attachment that was mentioned earlier. This is the ligament that gets damaged with AC joint injuries.
When this ligament is damaged, the shoulder will present with a “step deformity” and it is typical to have long-term pain associated with this injury, as well as the development of osteoarthritis in the years to follow.
The Transverse Humeral Ligament:
The Transverse Humeral Ligament is composed of some fibers from the subscapularis tendon as well as some fibers of the supraspinatus.
Unfortunately, this leads to the vulnerability of this ligament if one of those structures is ever compromised. This ligament holds the biceps within the bicipital groove.
If this ligament is ever damaged, you may notice some “snapping” in the front side of the arm. This typically indicates that the biceps tendon is no longer stabile within the bicipital groove.
Muscles of the Shoulder
Hopefully, you are very familiar with important muscles of the shoulder and their related tendons.
The rotator cuff muscles:
• the supraspinatus
• the infraspinatus
• the subscapularis
• the teres minor
The rest of the muscles (non-rotator cuff muscles):
• the teres major
• the rhomboids (major and minor)
• the trapezius muscles (upper, middle, lower)
• the latissimus dorsi
• the levator scapula
• the biceps (long head)
• the coracobrachialis
• the pectoralis minor
• the pectoralis major
• the triceps (long head)
• the deltoid
Muscles of the Trunk
Proper function of the trunk, more commonly referred to as the “core,” is critical to the prevention and/or rehabilitation of rotator cuff tears.
The general rule of thumb is this: without a strong core, you cannot transfer energy from the lower body (from the windup) to the upper body.
Some muscles of the trunk to know moving forward are:
• the internal oblique
• the external oblique
• the rectus abdominis
• the transverse abdominis
• the quadratus lumborum
• the multifidus
• the paraspinalis
• the lumbosacral fascia
Shoulder Stabilization
What we are about to discuss is some pretty technical stuff.
Please feel free to skip ahead if you do not care to dive in to it. This is more intended for those of you who have spent at least a year in an anatomy course.
Due to the naturally shallow bony configuration of the glenohumeral joint, the shoulder is an extremely unstable joint.
Stabilization in the joint is relative and is linked to the beautifully choreographed dance between the static and dynamic stabilizers.
Passive and active soft tissue structures provide the joint with enough stabilization to move it through a large range of motion. Passive stabilization of the glenohumeral joint comes from the entire inferior glenohumeral ligament, the coracohumeral ligament, the anterior band of the inferior glenohumeral ligament, the combined superior and middle glenohumeral ligaments, negative internal pressures, and the glenoid labrum.
The superior shoulder capsule plays an important role in passive stability of the GH (glenohumeral) joint. A tear in the superior capsule at the greater tuberosity, which can be seen with partial rotator cuff tears, significantly increases anterior and inferior translation.
A complete tear or void of the superior capsule, which is seen in large cuff tears, significantly increases glenohumeral translations in all directions. (58)
A study, conducted in 2005, noted the effects of different ligaments and muscles on GH external rotation in different positions: neutral, abducted at 15°, and abducted at 60°. The study found that GH joint acts as a cylinder and is supported by different anatomical structures in different positions of external rotation.
In a neutral position, the structures that provided resistance to external rotation (in order of greatest resistance to least resistance) were: the entire inferior glenohumeral ligament, the coracohumeral ligament, the anterior band of the inferior glenohumeral ligament, and lastly the combined superior and middle glenohumeral ligaments.
In a 60° abducted position, the muscles providing resistance to external rotation (in the same order as above) were: the entire inferior glenohumeral ligament, the anterior band of the inferior glenohumeral ligament, the combined superior and middle glenohumeral ligaments, and, lastly, the coracohumeral ligament.
Shoulder Movements
Motions of the Shoulder (GH Joint)
- Flexion – bringing the arm forward
- Extension – bringing the arm behind (opposite of flexion)
- Internal Rotation – with the arm elevated and elbow bent, the hand with drop towards the ground.
- External Rotation – with the arm elevated and elbow bent, the hand with move upward.
- Adduction – the shoulder moving towards your legs (toward midline).
- Abduction – opposite of ADDuction or your pant pocket. Basically raising your arm overhead but from the side (not flexion).
Motions of the Shoulder Blade
- Scaption – Motion in the Scapular plane (roughly 30 degrees forward).
- Upward Rotation – When the inferior angle of the shoulder blade flares outward way from the midline of the body.
- Downward Rotation – Opposite of upward rotation.
- Retraction – Moving the shoulder blades toward the spine, as if to flex the back muscles.
- Protraction – Moving the shoulder blades away from the spine. Similar to the Hunchback of Notre Dame.
- Elevation – Moving the shoulder blade up towards your ears
- Depression – Moving the shoulder blade down away from your ears
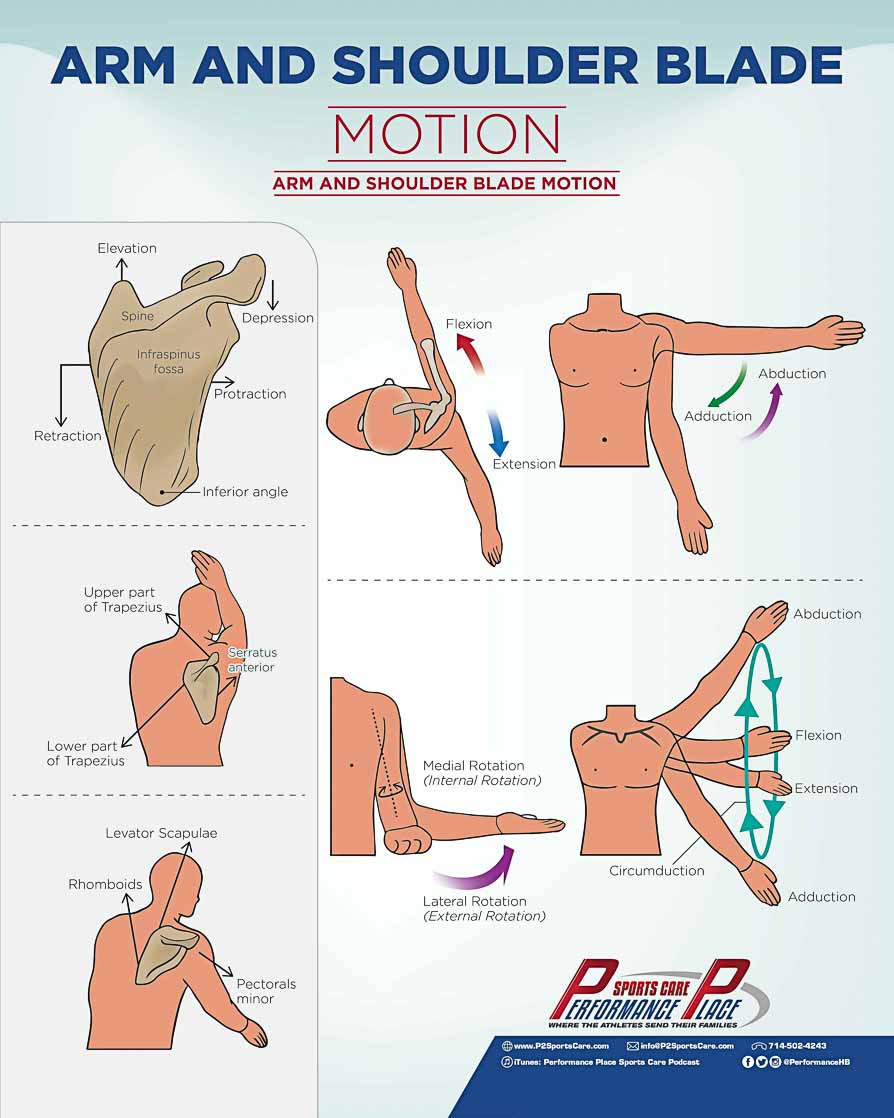
Share this Image On Your Site
NOTE: IF YOU ARE USING A DIVI WORDPRESS THEME YOU MUST EMBED IN THE CODE MODULE… NOT THE TEXT MODULE
How the Shoulder Works
Without knowing the basics of shoulder motion, you will not be able to fully understand the various functions of muscles and tendons.
Some of the best educational papers on ball and socket joints, like the shoulder, include these terms of motion.
In order to make the most of your education on the shoulder and the rotator cuff, you must fully understand these motions and commit them to your memory!
How to Understand the Function of the Shoulder Muscles
All of these muscles of the shoulder can be grouped into one of three categories based on their function. Think of the three P’s: (59)
1. Glenohumeral Protectors
2. Scapulohumeral Pivoters
3. Humeral Positioners (Propellers)
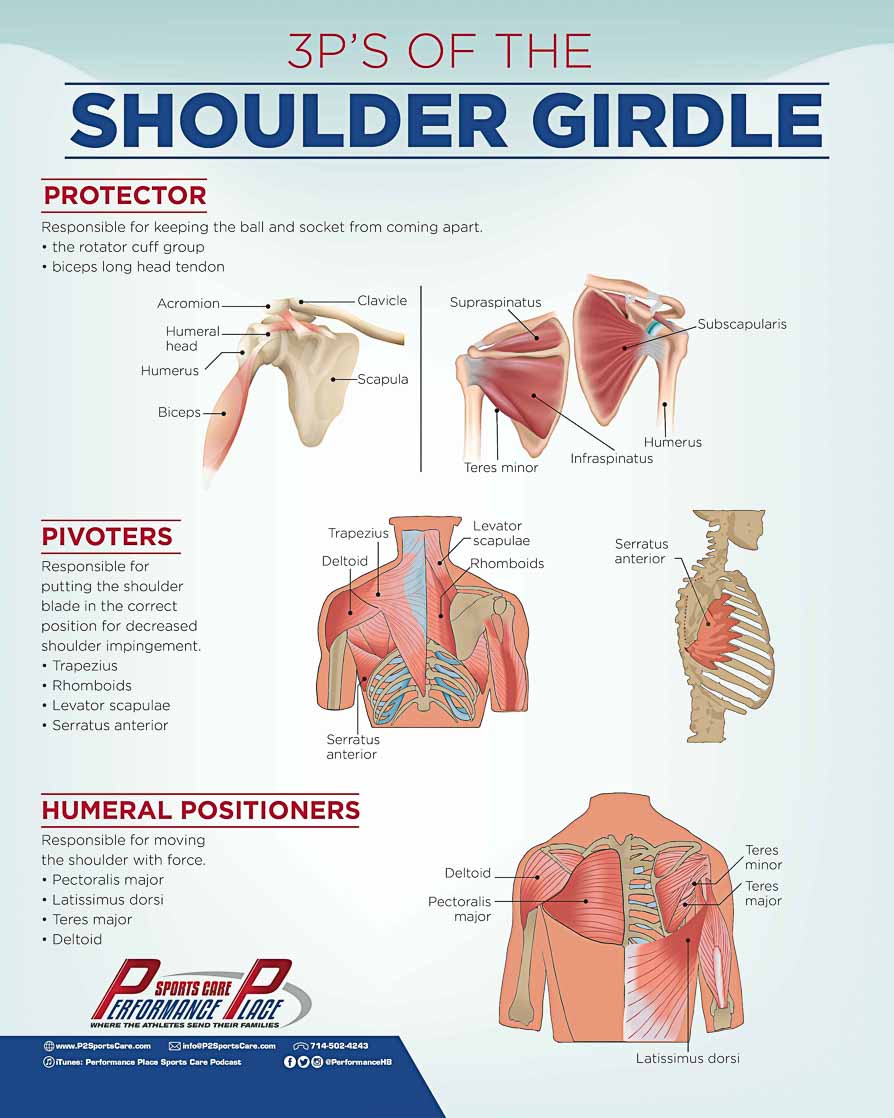
Share this Image On Your Site
NOTE: IF YOU ARE USING A DIVI WORDPRESS THEME YOU MUST EMBED IN THE CODE MODULE… NOT THE TEXT MODULE
Glenohumeral Protectors
The muscles grouped into this category are:
• the rotator cuff group
• biceps long head tendon
The rotator cuff muscles and the biceps long head tendon all have the job of keeping the glenohumeral joint (the ball and the socket) protected from coming apart.
The glenohumeral protectors are joined by the labrum and other ligaments in preventing shoulder dislocation during different ranges of motions and under different loads.
The glenohumeral protector muscles assist in keeping the joint intact via dynamic stabilization.
The rotator cuff provides a counteractive force to the humeral head moving superiorly (upward) during over-head shoulder motions.
If this downward pull did not occur, impingement would occur and then rotator cuff tears would follow. (6) Athletes with shoulder instability have also been shown to have poor firing patterns of the rotator cuff. (21)
Here are some great pictures.
The great thing about the rotator cuff is that, in optimal circumstances, it is really good at its job.
The subscapularis and the infraspinatus actually have the potential to generate more force than the posterior deltoid and the brachioradialis.
Every complete muscle/tendon has its optimal length and tension. We call this the “length-tension relationship.” The rotator cuff has a very narrow optimal range. The optimal range of the rotator cuff is created only when the shoulder blade is functioning well in combination. (50)
Habitually poor shoulder blade positioning, strength deficiencies, and poor movement patterns result in rotator cuff tears.
Scapulohumeral Pivoters
Muscles of this category are:
• Trapezius
• Rhomboids
• Levator scapulae
• Serratus anterior
This group of muscles is responsible for putting the shoulder blade in to the correct position to allow for proper functioning of the rotator cuff and also to decrease any amount of impingement on structures that lie underneath the acromion of the shoulder.
The area underneath the acromion is often referred to as the subacromial space.
This is where impingement will occur, but you can open up the space if you position the shoulder blade well.
The position of the shoulder blade is important because it is where the rotator cuff originates. If, during a pitch, the shoulder blade does not move with the humerus, then the rotator cuff would tear apart from being stretched on both of its ends.
Optimal position of the scapula is also needed for optimal centralization of the humeral head on the glenoid fossa (ball on socket).
While throwing, from the cocking phase to the follow-through, the shoulder blade will move between 15-18mm, from retraction to protraction respectively.
During flexion and abduction of the shoulder (raising the arm above the head), the deltoid is not the only functioning muscle.
The trapezius (upper, middle, and lower) and the inferior fibers of the serratus anterior all function to guide the shoulder blade into the correct position for complete, pain-free, unrestricted range of motion.
• Scapulohumeral rhythm – rotates about a fixed axis of 65 degrees.
Humeral Positioners
These muscles are the ones that can generate a lot of force and energy. Some muscles in this category are:
• Pectoralis major
• Latissimus dorsi
• Teres major
Typically, in a rehabilitation setting, these are the last to be focused on.
Strengthening of the protectors and pivoters comes first, so that when the rapid motion generated by the humeral positioners is added in to the equation, the joint is well-supported.(19)
WINDUP MECHANICS
What Muscles Are Working During a Pitch?
The muscles of the body need to work together in order to do the job right. Muscles of the leg and hips are primarily responsible for creating a stable base that the muscles of core can rotate and flex upon.
After this phase of throwing, assessing the quality of movement becomes difficult because of how quick the motion is.
The average time it takes for the ball to be released from the pitcher’s hand after the front foot makes contact with the mound is 0.145 seconds. (45)
The two motions of the body that allow for the best acceleration of the ball and pitch velocity are:
- A large amount of external rotation of the shoulder
- Forward, linear trunk motion (35)
The pitching motion is often broken down into 6 phases: (43)
1. Windup
2. Early Cocking/Stride
3. Late Cocking
4. Acceleration
5. Deceleration
6. Follow Through

Share this Image On Your Site
NOTE: IF YOU ARE USING A DIVI WORDPRESS THEME YOU MUST EMBED IN THE CODE MODULE… NOT THE TEXT MODULE
Windup Phase
The wind up begins with the hind leg stance. The lead leg is raised to its highest point and the separation of the hands.
In order to achieve an optimal windup, your center of gravity must be kept over your back foot. If this is not done, you will drift/“float” to the plate.
Keeping your center of gravity over your back foot will allow for maximum power and velocity on the ball.
Windup Tip: Falling forward prematurely, during the windup, requires the shoulder to work a lot harder for the same velocity you would get if you did not fall forward prematurely. (4,10)
Early Cocking/Stride Phase
Early Cocking/Stride is defined as the phase that begins when the ball leaves the glove and ends when the front foot hits the ground.(43)
During this phase, the pelvis will achieve its maximum rotational velocities of 400 to 700 degrees per second. (11) The purpose of this stride is to create the potential for the trunk to assist more in the velocity of the pitch.
Remember, forward, linear trunk motion is number two on the list of most important body motions that create ball velocity.
Early Cocking/Stride Tip: Achieving a longer stride will allow for more trunk activation while pitching, however, a stride that is too long will decrease the amount of energy generated from hip rotation.
Here are the highlights during Early Cocking/Stride. (43)
- Shoulder external rotation begins:
- Via the parts of the rotator cuff (supraspinatus, infraspinatus, and teres minor)
- Occurs late in the phase
- The shoulder blade positions itself in upward rotation and retraction
- The muscles of the shoulder blade accomplish this to create a stable base for shoulder rotation
- Via the middle trapezius, rhomboids, levator scapula, and serratus anterior
- Adduction of the shoulder
- The deltoid shortens early in the phase to accomplish this
- Pelvic rotation begins (47)
- Abdominal obliques limit low back hyperextension
- Motion toward the plate creates inertia related hyperextension
- Gluteus maximus stabilizes the pelvis for trunk motion
Late Cocking Phase
Late Cocking is the period between the front foot making contact with the ground and the maximal point of external rotation of the throwing shoulder.(43)
Late Cocking is a critical phase for rotator cuff health, mainly because the supraspinatus is in an extremely vulnerable position, especially if the correct amount of space in not preserved in the subacromial space of the shoulder.
Late cocking requires humeral abduction of 80° to 100°, which the optimal range for impingement of some of the tendons of the shoulder to occur or for a bursa to development.
Proper shoulder blade function will resolve this via upward rotation and elevation.
The most commonly torn muscle of the rotator cuff group is not extremely active in this position required of the late cocking phase. However, the job of this muscle and of the biceps long head tendon is still very important! These two structures compress the ball and the socket together and if they are not working properly in the “late cocking” position, the shoulder could feel “loose.” (31)
This externally rotated position proves to be an extreme advantage in increasing ball acceleration. The more external rotation a pitcher can achieve at the end of the late cocking phase, that is still safe and reasonable, the more distance the body has to increase the acceleration of the ball through the pitching motion.
An analogy that may assist you in understanding this is bobsledding. If the bobsledding team has a longer runway to sprint with the sled before they need to jump in, they then have more time to accelerate the bobsled, and the sled will therefore travel through the course much faster.(46,55)
Here are some highlights!
- Humeral Head depression:
- Via supraspinatus
- Humeral Head compression into the socket:
- Via supraspinatus
- Shoulder Blade retraction and upward tilt:
- Via middle trapezius, rhomboids, and levator scapula
- Shoulder is adducted and attains maximal external rotation:
- Via infraspinatus and teres minor
- End of external rotation is found via shortening contraction of the subscapularis, pectoralis major, and the latissimus dorsi.(7)
- Maximum internal rotation torque at the end of maximum external rotation (9)
- Pelvic rotation is at a maximum (47)
- The trunk accelerates forward and laterally:
- Loading of the core muscles (47)
Acceleration Phase
The acceleration phase of the wind-up is defined as the part of the pitching motion that begins with the shoulder at its point of maximum external rotation and ends with the ball being released. (43)
This phase is characterized as a drive to the plate. Many of the actions that the body was just doing are now being “reversed.” The rapid change in direction creates a huge amount of torque force on the shoulder and the elbow as they move in to the end of the phase.
Anytime a joint or muscle/tendon changes direction, it can potentially become damaged, especially if was not in good health to start with.
Even when the shoulder blade changes direction, it must still continue to be a stable platform for safe rotation of the shoulder joint. For this reason, the shoulder blade must be well-trained (this is a whole tangent topic, see scapular stabilization exercise).
The elbow becomes extended, first, by the momentum the trunk creates while accelerating to the plate, and, second, by the shortening of the triceps. Internal rotation of the shoulder comes just after the elbow reaches its maximum extension and is meant to protect the elbow from torqueing damage.
Are you thinking ulnar collateral ligament injury?
You are on the right track!
Although this article talks specifically about rotator cuff tears in pitchers, poor mechanics can create a variety of injuries in the joints while pitching.
Interestingly, during this phase, the pelvis is angled anteriorly (aka anterior pelvic tilt) to create more distance to accelerate the ball.(46, 55) Remembering that bobsled analogy right about now?)
The reason this is so interesting is because in general population strength training and core exercise, most fitness professionals will attempt to train an athlete in a neutral pelvis position. Anterior pelvic tilt, however, will typically create an increase in low back extension.
If pitchers are going to live in lumbar extension, then why not condition them to control their body better in that position?
I am willing to bet that most of you reading this article are interested in learning more about increasing the velocity of the ball before release. Remember, we have to have more contact time with the ball in order to accelerate it faster.
Two things that only take a short period of time to accomplish, and most pitchers can improve on during the acceleration phase are:
- More trunk flexion
- More lead knee bend
One thing that cannot be improved quickly is increasing external rotation of the shoulder. Trying to achieve this in a short period of time should NOT be attempted.
The shoulder changes over time and will change its structure in order to adapt to pitching. Trying to increase the speed of this process is a recipe for disaster as far as I am concerned.
Here are the highlights!
- Shoulder blade protraction:
- Via serratus anterior (12)
- Provides a stable base for safe and quality internal rotation towards the plate (31)
- Forces of the shoulder change from eccentric (lengthening contraction) to concentric (shortening), dominating on the front side. (34)
- Pectoralis major, latissimus dorsi, subscapularis, serratus anterior
- Forces of the shoulder change from concentric (shortening contraction) to eccentric (lengthening), dominating on backside. (34)
- Maximum internal rotation of the shoulder after ball release (29)
- Maximum elbow extension achieved at ball release (29)
- Trunk forward flexion and lateral tilt away from throwing arm:
- More knee flexion on the leading leg improves the stability of this point for more trunk flexion/rotation which amounts to more velocity (29)
Deceleration Phase
The deceleration phase of pitching is defined as the time between the point that the ball is released and the point of maximum internal rotation of the shoulder and maximum elbow extension. (43)
It is known as the most violent part of the pitching motion, much like slamming on the brakes before hitting another car; it happens fast.
Which structures take all of the beating of this phase?
In general terms, it is the backside of the shoulder. More specifically, the structures that take the beating during this phase are the infraspinatus, teres minor, and the posterior deltoid.
Here are the highlights!
- Extreme backside rotator cuff deceleration (12)
- Teres minor, infraspinatus, and posterior deltoid slow the majority of the acceleration force.
- Extreme load on the biceps tendon (12)
- Slows the elbow extension and pronation of the forearm.
- Extreme load on the shoulder blade muscles (12)
- Trapezius, rhomboids, and serratus anterior slow forward motion of the blade.
Follow Through
The follow through continues up until the body stops.(43) Since everything is progressively slowing in speed at this point, there is a low likelihood of injury. Typically, if an injury is sustained in this position, it would come from a ball that was hit back at you. You can, of course, avoid this by being in proper fielding position.

Share this Image On Your Site
NOTE: IF YOU ARE USING A DIVI WORDPRESS THEME YOU MUST EMBED IN THE CODE MODULE… NOT THE TEXT MODULE
Partial-thickness tears are exactly what they sound like: they do not extend all the way through both surfaces of the tendon. If it makes it easier to visualize, think of drilling/ cutting a hole only partially through a piece of wood. The hole begins on one surface of the wood, but does not go all the way through to the opposite surface.
Full-thickness tears are just the opposite: these tear goes all the way through to both surfaces of the tendon. There are, however, two different types of full-thickness tears to be aware of.
The less severe of the two types of full-thickness tears is called and incomplete, or focal, tear. This type of tear is still a “through-and-through” tear, but it does not compromise the entire tendon.
Think, for example, of a drilling a hole through a wooden dowel. The hole is “through-and-through” and goes from one surface to the other, but it does not cause the wooden dowel to break.
The second, and more severe type of full-thickness tear, is called a complete, or full tear. In complete tears, the tendon is completely torn through both surfaces. The tendon becomes detached and, often, retracted to varying degrees. The more the tendon is retracted, the less successful surgical intervention is expected to be.
Location of the tear can then be used to better describe the rotator cuff tear:
• Bursal
• Articular
• Intrasubstance
Bursal side partial tears are classified as such when the tear extends from the bursal surface of the tendon down to the attachment site.
The bursal side is the more superficial side of the rotator cuff; adjacent to the deltoid. Bursal side partial tears do not extend all the way through to the articular side (undersurface), otherwise it would be a full-thickness tear.
Tears on the articular side of the cuff will commonly occur anteriorly on the supraspinatus; at the distal attachment site to the greater tuberosity.
These types of tears are especially common in the under 40 population.
Intrasubstance tears are classified as partial thickness tears that extend to neither the bursal side OR the articular side. Though these tears do not immediately present themselves as being equally as severe as the other two tears mentioned above, they are often found to be precursors to a much larger tear in the future.
Rotator Cuff Diagnosis
Common symptoms include:
• Pain on the front side of the shoulder (during throwing and/or rest)
• Pain while sleeping (even if not laying on the affected side)
• Loss of strength and/or motion
Properly diagnosing a rotator cuff tear usually includes orthopedic testing and diagnostic imaging. Until the region is properly tested, there are still a number of possible conditions that could account for the symptoms that the pitcher is experiencing.
The following is a list of the top, possibly present conditions:
1. Subacromial Impingement
2. Subacromial Bursitis
3. Shoulder Labral Tear or SLAP
4. Glenohumeral Instability
5. Rotator Cuff Tendinopathy
Note that many of these shoulder diagnoses can overlap and even though they are referred to by different diagnoses, they can sometimes even be different grades of the same condition.
It is extremely common to see impingement, bursitis, tendinopathy, and instability result from a rotator cuff tear.
Think of a sports care that has a loose wheel. If you were to continue driving the car despite its loose wheel, it will wreak havoc on the rest of the car. The tire, the wheel, the wheel well will all get absolutely destroyed if more miles continue to be driven without fixing the loose wheel.
Think of the shoulder joint in the same way: when something within the joint is damaged, loose, or whatever, the rest of the structures around the one that was initially damaged, will become negatively affected as well.
For this reason, I try to not tell a pitcher what their diagnosis is.
It makes no difference if the case is a rehabilitation case or a surgical case: the process of strengthening the rotator cuff, the shoulder girdle, the core, the hips/legs, and of speaking with a pitching coach in regards to the mechanics of that pitcher will remain, fundamentally, the same.
Rotator Cuff Orthopedic Testing
All orthopedic tests used to identify possible rotator cuff tears have different ranges of sensitivity and specificity, and can usually lead to a primary diagnosis of a Rotator Cuff Tear.
However, the primary diagnosis cannot be confirmed until there are diagnostic images to support it.
Below, you will find a list of words and definitions that you will need to know if you are hoping to understand orthopedic testing and imaging modalities.
- Sensitivity:
- A sensitive test helps rules out a diagnosis (when the result is negative).
- Specificity:
- If a test has a high specificity, the diagnosis is ruled in with a high degree of confidence.
- Positive Predictive Value:
- If the test result is positive and there is a high value, there is high probability that the patient actually has the pathology/diagnosis.
- Negative predictive value:
- If the test result is negative and there is a high value with it, there is a high probability that the patients does not have the pathology/diagnosis.
Mechanism of Injury
The late cocking phase has been referred to as the “critical point” for possible injuries of the shoulder, specifically in the superior labrum and the rotator cuff.
The position of the late cocking phase requires the shoulder to be at its point of maximal external rotation. The forces acting on the glenohumeral joint, at this point, are very strong and are coming from different directions.
The forces are so strong, in fact, that the humerus will actually begin to remodel itself after so many pitches have been thrown. This adaptation occurs in the humerus in order for it to adapt to the forces required in external rotation.(5, 32, 39)

It is during the late cocking phase that the labrum appears to be under the highest amount of strain. The strain in this position is so high that human cadavers in a lab setting actually presented with SLAP lesions after being put in the late cocking phase position.(24, 36, 44)
As far as rotator cuff tears are concerned, the theory is that high-compressive loads combined with shoulder impingement will create articular side tears during this phase.(17, 52)
Another theory is that the high external load is too much for the rotator cuff to handle and will then create capsular torsion. (22,42)
Assessment of a Rotator Cuff Tear
Assessing the whole body is critical in correcting the mechanism of injury in rotator cuff tears in pitchers. Assessment is necessary in each of these areas:
1. Kinetic Chain Functioning
2. Evaluation of the Shoulder Blade
3. Glenohumeral Rotation (External, Internal and Total)
4. Orthopedic Testing
5. Special Imaging
1: Kinetic Chain Functioning
The kinetic chain is just a fancy term we use to refer to the connection between different parts of the body.
In pitching, a 90 mph fastball is delivered to the plate with proper functioning of the legs, hip, trunk, shoulder blade, shoulder, elbow, and wrist.
If one part of this “chain” is injured, weak, or not being used well, then the speed of that fastball will decrease. The kinetic chain is the link between the different parts of the body.
Assessment of the kinetic chain can be performed in a variety of ways. I would strongly suggest the use of more than one of these methods to confirm any findings. Typically, if the kinetic chain breaks down in one region, then a rehabilitation program will be prescribed in order to address the specific issue.
Example of a kinetic chain breakdown:
The legs are not being used to drive towards the plate.
Possible reasons:
- Injury to a joint/muscle/tendon of the foot, knee, hip, or trunk
- Poor pitching mechanics
- Poor single-leg stabilization (drifts to plate due to lack of balance)
- Low-leg/hip/trunk strength
As you might be able to see with the above list of possible reasons for the stated kinetic chain breakdown, the type of correction required would depend upon the actual reason for the breakdown.
Perhaps, the pitcher’s poor mechanics are a result of never having received proper instruction, or maybe low strength levels come from never having lifted properly; you get the point.
2: Evaluation of the Shoulder Blade
In addition to assessing the shoulder as part of the kinetic chain, it should also be assessed individually.
The shoulder blade has the huge responsibility of creating a direct, stable base for the ball and socket of the shoulder to rotate.
If this stable base does not exist, then the rotator cuff has no chance of surviving into college.
So, what are we looking for when we evaluate the shoulder blade?
I like to start with Static (resting) and Dynamic (movement) of the scapula.
- Is there symmetry between sides?
- Does one side wing?
- Does one side elevate?
In the resting position, the medial (inward) border of the shoulder blade should be parallel to the spine but the dominant side often appears further away from the spine.
Assessment at rest should be in three positions:(59)
1. Seated with arms hanging at the sides
2. Seated with hands on hips
3. Seated with arms abducted to 90 degrees
During motion assessment we would for:
• Scapular winging
• Premature elevation & protraction
• Unsmooth motions
• Rapid downward rotation when the arm is lowering
These are all easy to see but do not always mean you have pain, however I would not be surprised if a year from now you develop some shoulder pain.
There are more ways to assess the shoulder blade but to keep this section short I decided not to include them.
3: Glenohumeral Rotation (External, Internal, and Total)
Assessing the rotational range of motion is pretty standard among rotator cuff assessments. The athlete should lie on their back with their upper arm out to the side (perpendicular to the rest of the body) and a 90° bend at the elbow.
The range of motion measurements are taken with an instrument called a goniometer. The numbers are recorded and the left and right sides are compared.
Ideally, the rotational range of motion measurements should be taken every season, or every other season.
If a pattern of decreased range of motion is noticed, their stretching and eccentric exercise programming needs to be adjusted accordingly.
As a pitcher, there will be more laxity in the glenohumeral joint. Or, to sound a little less technical, pitchers have a looser ball and socket shoulder joint than the average person. Usually, pitchers tend to have more external rotation in the joint than internal rotation.
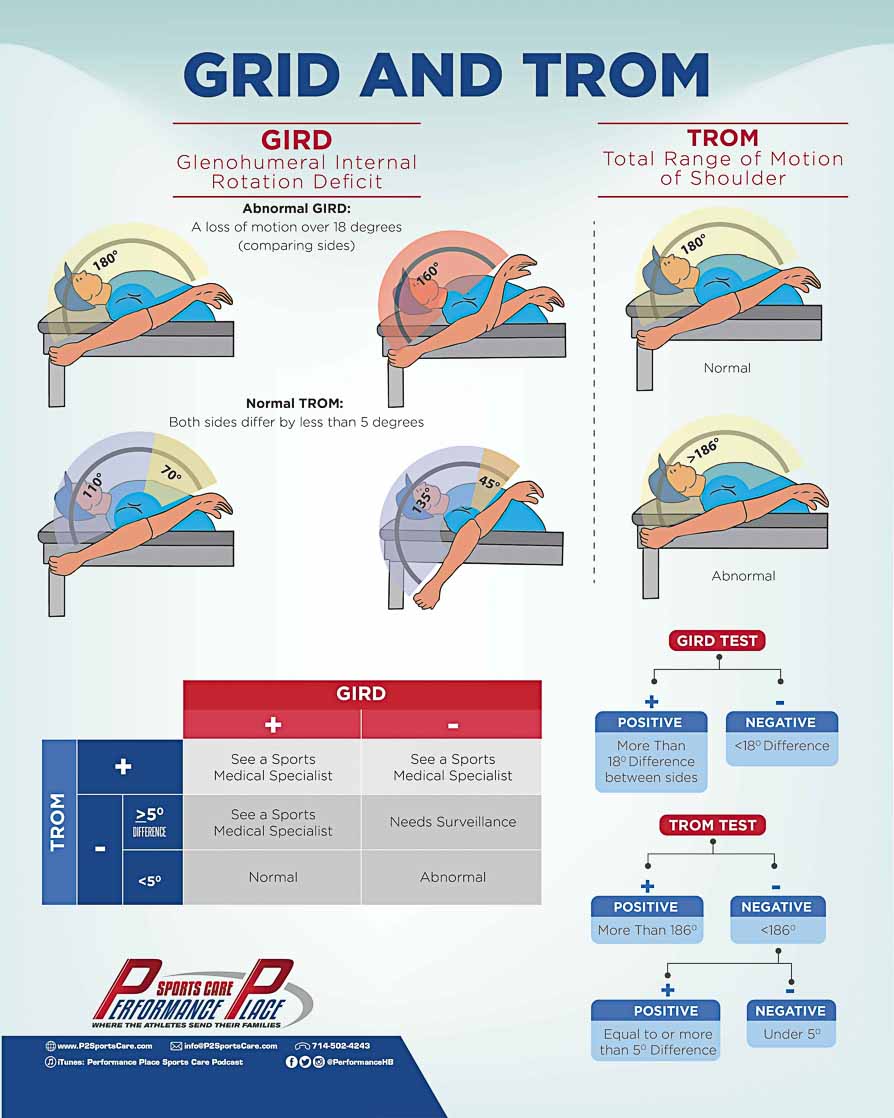
Share this Image On Your Site
NOTE: IF YOU ARE USING A DIVI WORDPRESS THEME YOU MUST EMBED IN THE CODE MODULE… NOT THE TEXT MODULE
Gains of more than 5° in external rotation of the throwing arm are considered normal in pitchers. This gain in range of motion is considered so normal, in fact, that if a pitcher does not have this increase, then they would actually be considered deficient in external rotation. External Rotation Deficit (ERD) is when less than 5° range of motion is gained in the throwing arm of a pitcher.
Glenohumeral Internal Rotation Deficit, or GIRD, refers to a loss of range of motion in the shoulder during internal rotation.
GIRD is defined as a difference of 18-20° between the throwing arm and the non-throwing arm. The throwing arm would be the arm presenting with the loss of internal rotation.(20, 28)
In the past, it was believed that a difference of more than 18-20° was considered pathological, and anything less than that was considered normal.
However, recent research actually shows a number greater than 18° is only bad if it is combined with a los of total range of motion (TROM) by more than 5° between both arms is significant.
Having GIRD can make a pitcher 1.9 times more likely to sustain a shoulder injury. (53)
I know it’s confusing… this is why I created an infographic about the topic. This could be one of the most important bits of information you could share with your teammate, so please SHARE.
Here are the indicators that we know to be dangerous given the research available at this time:
- GIRD greater than 18-20° with a loss of 5-8° in TROM
- TROM cannot exceed 186° (20, 28)
What can cause these changes in range of motion?
- • Bony changes, especially in pre-pubescent athletes (5, 31, 32, 38)
- Capsule/ligament thickening from scar tissue build-up after repetitive tensile loads (3,49)
- Repetitive muscular strain leading to an increase in muscle stiffness (37, 56)
4: Orthopedic Testing
Orthopedic Tests are tests that are designed, specifically, to identify the presence of torn, frayed, irritated, and/or broken structures, and also to identify what structure is damaged.
In the world of Sports Medicine, these tests are a standard or practice. Any doctor you see, will perform these tests in order to reconfirm the working diagnosis of other doctors.
Some of the most common Orthopedic Tests are listed below, along with the structure(s) they are used to test and their relative usefulness.
- Muscle Testing for the rotator cuff
- Supraspinatus Test (Empty-Can Test)
- Tests for supraspinatus impingement or the integrity of the supraspinatus muscle and tendon
- Supraspinatus Test (Full-Can Test)
- Supraspinatus pathology
- If Empty-Can Test is positive, but Full-Can is negative this indicates that the shoulder pathology is not primarily an RC lesion.
- Codmen Drop-Arm Test
- 10% sensitivity, 100% specificity (54)
- Lift-off test
- Tests for subscapularis rupture
- Palpation for defect
- 96% sensitivity 97% specificity (57)
- External Rotation Lag Sign
- 100% sensitivity and 100% specificity for stage 3 and stage 4 fatty degeneration of the infraspinatus on an MRI (51)
- Hornblower’s sign
- 100% sensitivity and 93% specificity for stage 3 and stage 4 fatty degeneration of the teres minor on and MRI (51)
- Dropping Sign
- Infraspinatus pathology
- Internal Rotation Lag Sign
- Subscapularis pathology
Special Imaging For The Shoulder
The following are the various types of imaging techniques you will hear being referenced as you proceed on this rotator cuff tear adventure:
• Plain radiograph (x-rays)
• Computed Tomography Scan (CT Scan)
• Magnetic Resonance Imaging (MRI)
• Magnetic Resonance Arthrogram (MR Arthrogram)
• Musculoskeletal Ultrasound (MSMU or MSKUS)
Plain radiograph (x-rays)
When you start to go down the path of imaging, X-rays are the most common starting point for a variety of reasons. X-rays are great at assessing the cortical surfaces of bones (the outer shell of the bone) and the alignment of bone structure. They can also help in raising suspicion of soft-tissue damage.
For example, with a groin pain case, we may see:
• Bone Spurs
• Local fractures (new or old)
• Bone disease
• Arthritis

Everything x-rays are able to see, however, are only a small fraction of what other types of images can see in many areas of the body, specifically in the shoulder region.
In order to completely and properly assess the muscles, tendons, ligaments, fascia, cartilages, and other structures of this region, we need to use imaging techniques that are better equipped to key in on those particular densities.
Computed Tomography Scan (CT Scan)
CT scans are extremely useful for more in-depth evaluations of bone injuries. CT scans will typically show the same structures that an x-ray will show, but in much greater detail.
So then, why not just start with the CT scan in the first place?
Well, for one, cost is a huge factor in why we do not. In the field of medical professionals and establishments, we try to make every attempt to keep the cost as low as possible for every patient.
Unfortunately, even despite our efforts, imaging can often be one of the fastest ways to make your medical bill skyrocket in an attempt at finding answers.
The machinery used to create images for CT scans is not only very expensive, but it is also much more complicated than x-ray equipment, so it takes a little more time to produce a useful image. X-rays produce a useful image much faster than a CT scan and at a fraction of the cost.
Additionally, one of the biggest hang-ups of using a CT scan too early in the process is the amount of radiation. It is fairly common knowledge that exposure to radiation is not a good thing for us humans. However, we did not always know that.
At the time that x-rays were invented, doctors and medical professionals actually found radiation “helpful” in treating some skin conditions!
Needless to say, we have since come to very different conclusions on these so-called “benefits” of radiation, and because of that, each patient under medical care is limited to a certain amount of radiation exposure every year. Some estimate that CT scans have around 100 times more radiation exposure than x-rays.
Keeping with the same example of groin pain, a CT scan would be useful in showing:
• Stress Reactions (note that a stress reaction is not the same as a stress fracture)
• Inflammatory processes
Magnetic Resonance Imaging (MRI)
An MRI is very useful in evaluating the soft tissues of the shoulder. Using an MRI also allows us to better predict recovery time for the injury and to create a more precise treatment plan for the patient.
Having this type of image available allows us the opportunity to greater understand the simplicity or the complexity of the rotator cuff tear. It also assists us in being able to rule in or out some aspects of the injury and confirm others.
Some conditions of interest that an MRI would work very well to display on an image are:
• Muscle strains
• Tendon injuries
• Stress reaction
• Subacromial Impingement
• Frozen Shoulder
• Labral tears
• Bursitis
Though MRIs are excellent in the quality of image and in what they help us observe, that quality comes at a high price. MRIs are not cheap, and the image is also not produced as quickly as an x-ray.

If you feel as though the cost of the image is worthwhile, you could likely go out and have an MRI performed on your injury today!
With the three images that we just went over, is there any need for the other types of imaging techniques? No, probably not.
X-rays and CT scans are great for bony evaluations. An MRI is great at evaluations of the soft tissues not found on x-rays or CT scans, and pretty darn good at bone as well.
If you happen to be waiting on your insurance company to approve you for an MRI, I wouldn’t get your hopes up too high. There are some cases that can see a fairly quick turn-around with MRI approval, but the majority of cases going through insurance are not so lucky.
Sometimes it can take months to see any progress or approval: months of downtime, uncertainty, and pain.
In my opinion, these are huge downsides, especially while you are waiting on someone else to approve your care.
If you find yourself in this situation, you might want to think about how badly it is that you want to know about your possible rotator cuff tear.
How badly do you want to play again this year?
If your answer to these questions was, “I want to know about the tear really bad and I want to play again this year,” then pay the money for the MRI.
Don’t allow money to be the barrier between you being happy and sane or you being bummed, confused, and irritated. An MRI is expensive, but it is money well-spent.
You might be wondering if the MRI is the most cost effective imaging technique for confirming the reason for your shoulder pain.
Well, actually it isn’t.
I don’t want to send the impression that I am trying to convince you to pay money to get an MRI. But I will say this, based on my experience since being in practice, I have found that people will often use money as the reason why they cannot get quality care and/or imaging for their injury.
However, most of the people that say money is the barrier, are the same people that come in with the latest and greatest version of other luxuries.
Personally, I take this opportunity to speak openly with these patients about prioritizing their health and quality of life above new gadgets and other temporary pleasures.
Unfortunately, too many people don’t realize or appreciate the value of a pain-free, healthy life until they have experienced life with chronic pain or chronic health issues.
What do you value most in life? Your health or the other stuff?
Let me go ahead and step off my soapbox. Let’s get back to the imaging!
Magnetic Resonance Arthrogram (MR Arthrogram)
MR Arthrograms are the gold standard in evaluating the interior anatomy of the shoulder (internal inspections usually imply a labral tear). Rotator cuff tears and labral tears can present independently or together. The rehab for labral tears is much harder and longer than rotator cuff rehab.
If you notice that in your rehab for your shoulder, you are progressing slower than what is expected, a doctor or medical professional might suggest an MR arthrogram to investigate the possibility of a labral tear.
The use of contract dye in the MR Arthrogram is what makes this image more expensive than a standard MRI. The dye will inflate the joint spaces and create a great visual for the structures inside of the shoulder joint.
Musculoskeletal Ultrasound (MSUS or MSKUS)
Last, but certainly not least, there is the Musculoskeletal Ultrasound. The MSUS is a newer form of technology compared to the previous imaging techinques mentioned in this article. One major upside to this form of imaging is that it is the most cost effective.
In other words, it is the biggest bang for your buck. It works great for identifying soft-tissue injuries, but it lacks the ability to see bony damages well, or at all.
What exactly can it see?
The MSUS can see pretty much everything that an MRI can see, yet orthopedic surgeons will often request an MRI over an MSUS. MRIs are a widely-used and a well-established tool in the medical world. Doctors may be attempting to stay with an imaging technique that they are very familiar, especially since they are making such a huge judgement call: the type of surgery that needs to be performed.
Over the recent years, MSUS has improved drastically. It currently is just as sensitive and specific as MRIs in what it picks up for the image, and it is only a fraction of the cost or MRIs.(33)

Over the recent years, MSUS has improved drastically. It currently is just as sensitive and specific as MRIs in what it picks up for the image, and it is only a fraction of the cost or MRIs.33
MRI: MSUS:
Sensitivity: 85.5% Sensitivity: 85.1%
Specificity: 90.4% Specificity: 92.0%
My recommendation for a comprehensive study package for shoulder pain would be this:
- An x-ray series to rule out any bony injuries
- An MSUS to rule in any soft tissue damage, including a rotator cuff tear.
Ultrasounds are the only type of image in the bunch that provides a dynamic assessment of the joint. This allows us to study the shoulder in motion! The dynamic aspect can help reveal other issues of the joint and can be instrumental in the prescription of specific treatment plans.
One very important thing to keep in mind with MSUS, however, is that the education and experience of the person performing the exam can create variability in the quality of the images. MSUS is a user dependent device, so the effort should be made to find a specialist who is qualified to perform the examination.
Not sure where to find a qualified individual who can perform MSUS?
Ask around!
Finding a qualified and experienced individual can be tough. Basic education in Sonography School is usually not enough to perform the exam, but, on the bright side, schools are beginning to add more musculoskeletal examination into their curriculum.
If you are in the Southern California area, two great people that I respect greatly are Dr. Michael Meng in the San Diego area and Michael Jablon in Beverly Hills.
Rotator Cuff Tear Treatments
The appropriate treatment for rotator cuff tears will depend upon the grade of the tear. If you do not know the grade, there are common routes to take to get started.
Each method of treatment has varying degrees of effectiveness, and as an added disclaimer; my inclusion of these methods in this list and in this article, in no way represent or symbolize my endorsement of these.
Each of these treatments have the potential to yield great results, if done correctly. However, there is always the other side of that, which would yield no results if done incorrectly.
• Rest
• Ice
• Activity modification
• Deep-tissue massage
• Electrical stimulation
• Therapeutic ultrasound
• Stretching activities
• Strengthening exercises
• Movement pattern activities
• Chiropractic manipulation
• Acupuncture
• Injections

Rehabilitation Of The Rotator Cuff
The mandatory goals of every rehab program are:
1. Decrease GIRD
2. Achieve less than 5° difference in TROM between sides, but keep it under 186°
3. Address scapular dyskinesia
4. Address kinetic chain deficiencies
GIRD and TROM rehabilitation
Range of motion in the glenohumeral joint (internal, external, and total), the shoulder blade excursion, and spinal mobility must all be assessed. Strength and flexibility of the muscles that attach the shoulder complex (the arm and the shoulder blade) to the body on both the front and the back need to be assessed as well.
A great way to start, is to increase the length of the muscles attaching the front side of the shoulder blade: the pectoralis minor and the short head of the bicep.(2)
If these muscles are not lengthened and remain tight, it will likely result in the shoulder blade being pulled forward and upward, and that means poor placement of the shoulder blade.
Basic mobilization with doorway stretching or myofascial release are great places to get started.
Scapular Dyskinesia Rehabilitation
This type of rehabilitation happens through a variety of movements, planes of motion, and effort levels. The shoulder blade moves through six planes of motion.
Typically, the goal is to improve the strength, endurance, and eccentric control of the scapular and shoulder muscles. For those types of exercises, there are many progressions.
Early activation of the weakened or “inhibited” muscles is critical in improving scapular positioning as well as scapular functioning. The muscles that are typically weakened are the middle trapezius, the lower trapezius, and the serratus anterior.(18)
There are progressions for exercises and positions that are meant to directly affect the function of these muscles.
Kinetic Chain Rehabilitation
Assessment of the kinetics chain include:
- hip-mobility
- leg-drive
- lower extremity strength
- dynamic core strength
- scapular stabilization
- rigidity in rotational power
These assessments are not to be taken lightly. It takes a trained eye and great coaching to be able to break years of bad habits in throwing and complex lower body motions, such as squatting and jumping.
Strengthening the athlete back to a great baseline level can take months or even years. Even small amounts of muscle growth cannot be seen until after 9 weeks of strength training at 4 or more days a week.
Most players, being that they are student-athletes or in-season at the time, will not be able to commit that kind of time to this training.
This is a great rehab program, to start in the off-season.
Changes in pitching mechanics can be seen in much shorter periods of time. Sometimes progress in pitchers can be seen in as short as a week! It is not uncommon, however, for pitchers to default back to old habits when they are not being coached in to better form.
In order to get the pitchers to form new habits, I have found that it takes more than a few months of hard work. It takes even longer when working with pitchers who are still growing.
As the length of the limbs change, the brain has a hard time keeping up. This is normal and is to be expected, so don’t get frustrated if this is what you are experiencing.
Rotator Cuff Surgery
As a general rule, surgery should be utilized only after extensive rehabilitation has occurred. The percentage of pitchers who are able to return to pre-op pitching levels, varies immensely.
If an athlete improves in GIRD, TROM, and scapular dyskinesia, yet is still experiencing pain while throwing, they will typically be a surgical case.
Regardless of the type of surgery, there are a few common objectives:
Debridement:
Remove any loose fragments of tendon, bursa, and anything else.
Making room:
Sometimes objects will get into the subacromial space and can cause more pinching on the rotator cuff. This will often require bone removal, called acromioplasty.
Reattachment:
Reattachment is done by suturing part of the tendon back together, or by reattaching the tendon to the bone.
Types of Rotator Cuff Surgeries
Arthroscopic Rotator Cuff Tendon Surgery
Arthroscopic repairs use a small camera/probe that is inserted into the shoulder joint through surgical incisions. The camera streams the views from inside the joint up on a TV screen for the surgeon to use as their guide in repairing the joint.
The surgical incision points used for arthroscopic surgery are usually very small, and since the tools and camera are not large, that is all that is really needed. When the tear is not very large, these types of procedures become possible.
Because only small points of entry are required of this type of surgery, it is considered one of the least invasive types.
Open Rotator Cuff Surgery
Open rotator cuff repairs were, actually, the first style of rotator cuff surgery. It is referred to as “open” because of the larger incision points required of this surgery.
This type of surgery is usually used on larger and more complex tears.
The cut will typically run about a few centimeters long right over the shoulder joint, right about where the deltoid muscle detaches. This will help them view the rotator cuff better during the procedure.
It is also common to perform this type of surgery when a full tendon transfer is being done. In addition to the tendon transfer, the surgeon may remove bone spurs around the acromion. The process of removing the bone spurs is called an acromioplasty.
Acromioplasty
Acromioplasty procedures are usually performed when the surfaces of the bones around the shoulder are irregular, specifically around the acromion process.
The goal of this procedure is to increase the amount of space between the bony process and the humerus that lies underneath.
When this is accomplished, the rotator cuff tendon and bursa between them will not get crushed while the shoulder is in motion. Acromioplasty can be performed during both arthroscopic surgery and open procedure.
Rotator Cuff Tendon Transfer
When the rotator cuff tear is so severe and calls for harvesting a tendon from elsewhere in the body to replace the cuff, then a rotator cuff tendon transfer procedure is performed.
Donor sites include the latissimus dorsi, and pectoralis major tendons. Trapezius muscle tendons have also started to gain popularity for this procedure.
The tear on the cuff should be so large, that the cuff is just considered unsalvageable in order to justify the use of this surgery. Choosing the donor tendon to replace the rotator cuff is a very important decision. The selected donor tendon could possibly change in the functions of that muscle-tendon complex.
Even though it is fairly unlikely that 100% recovery will be achieved after a surgery of this nature, 70-80% of your strength and functioning can be regained and that is a huge amount.(48)
If you are having this major procedure performed, I am sad to have to say that you probably will not be pitching again.
Rotator Cuff Surgery Recovery Time
The type of surgical procedure that you choose will dictate the time it will take you to recover after surgery. If you are a pitcher that requires surgery, you will more than likely opt for the arthroscopic option, especially if you are planning on returning to play.
Arthroscopic surgery has the shortest healing time and there is likely less damage that needs to be repaired since the incisions are so small.
Here is a brief timeline of functional recovery after surgery. This does not mean that the tendon is ready to throw again, it means that you feel better and starting moving well.
Let’s take a look at functional recovery, meaning you can function again.
• 30% functional improvement within 3 months
• 40% functional improvement in 3-6 months
• 30% functional improvement in 6 months and beyond (27)
When should you be throwing again?
That’s a whole different story.
Below are the success rates of various surgical procedures that are popular for rotator cuff tears: (14, 15, 25, 39, 40)
• Debridement: 16 – 85%
• Delaminations without repair to the bone: 89%
• Delaminations without repair to the bone: 33%
• Repair of a full thickness rotator cuff tear: 8% (25, 30)
Many pitchers struggle to throw at the same level that they were able to prior to the tear and surgery. This is mainly due to the development of anatomical changes within that shoulder over long periods of time of throwing at such a high level.
It was those anatomical changes that helped increase the strength and velocity of the throw that also lead to the injury.
When surgery is performed, the shoulder is restored back to normal anatomy and range of motion.
Normal, here, referring to the norm for an average human, and not the elite baseball pitcher who had superhuman external rotation and shoulder range of motion.
The restoration of the shoulder brings the pitcher back to a more “average” level, and often times they are unable to achieve the range of motion or strength that they had prior to surgery.
The pitcher also develops higher levels of joint laxity in the shoulder as a functional adaptation to their pitching.
Laxity is needed to be able to accelerate a ball through a longer range of motion. This will also need to be retrained after surgery.
For more information on how extra external rotation is important for high-velocity pitching, please revert back to the earlier section on early cocking, late cocking, and acceleration of a wind-up.
Conclusion
After reading an article this long, your head might be swirling with all this new information, and you might be asking yourself, “Ok, so what was the major take away here?”
Well, let’s try to simplify everything we went over.
If you are a pitcher with a rotator cuff tear, you more than likely have a breakdown somewhere in your pitching form, or there could also be a muscular imbalance somewhere that is causing your rotator cuff to work too hard.
Even if you go through rehabilitation for the rotator cuff, you are almost guaranteed to sustain the same injury again if you do not correct the lower body and the trunk.
Surgery should always be the final option, and some pitchers, unfortunately, should know that a surgery could mean not pitching again depending on the severity of the tear and the type of surgery selected.
If you are interested in seeing the route that I take with patients in our facility, we do have a free course for this.
I created a course because it blew me away that I was meeting so many pitchers who did not implement these research-based exercises in to their programs.
The exercises are simple, fast, and effective! They can’t have any benefit, though, if you don’t know what they are or what they do.
If you choose to access that course, and you enjoy the content on there, there is also a more advanced course that emphasizes the integration of the kinetic chain.
In this course, you can learn about core strength, lower body weight lifting, and power generation. Back when I was still playing, I wish I had had this information available to me. If you do not love this course, we will give you your money back.
For those of you that made it all the way to the end of this article, shoot me an email saying “FINISHED!”
I would love to chat with you and hear about your experience, and if this article was able to assist you at all in your pitching career.
Dr. Sebastian Gonzales DC, DACBSP®, CSCS, RMSK®
Huntington Beach CA 92648
http://www.P2SportsCare.com
References
1. Arthur, Rob. “At Least All These Tommy John Surgeries Aren’t Rotator Cuff Surgeries.” FiveThirtyEight. N.p., 27 Mar. 2015. Web. 04 Sept. 2016.
2. Borstad JD, Ludewig PM. Comparison of three stretches for the pectoralis minor muscle. J Shoulder Elbow Surg 2006;15:324-330.
3. Burkhart SS, Morgan CD, Kibler WB. The disabled throwing shoulder: Spectrum of pathology. Part I: Pathoanatomy and biomechanics. Arthroscopy 2003;19:404-420.
4. Burkhart SS, Morgan CD, Kibler WB. The disabled throwing shoulder: spectrum of pathology. Part III: The SICK scapula, scapular dyskinesis, the kinetic chain, and rehabilitation. Arthroscopy. 2003;19(6):641-661
5. Crockett HC, Gross LB, Wilk KE, et al. Osseous adaptation and range of motion at the glenohumeral joint in professional baseball pitchers. Am J Sports Med 2002;30: 20-26.
6. Reinold, Michael, Rafael Eascamilla, and Kevin Wilk. “Current Concepts in the Scientific and Clinical Rationale Behind Exercises for Glenohumeral and Scapulothoracic Musculature.” Journal of Orthopaedic & Sports Physical Therapy. N.p., 2009. Web.
7. Dillman CJ, Fleisig GS, Andrews JR. Biomechanics of pitching with emphasis upon shoulder kinematics. J Orthop Sports Phys Ther. 1993;18(2):402-408
8. Euler, Simon A., Dirk Kokmeyer, and Peter J. Millett. “Rotator Cuff Tears in Athletes: Part II. Conservative Management – American Mind.” Sports Injuries to the Shoulder and Elbow (2015): 57-62. Web.
9. Fleisig G, Escamilla RF, Andrews JR, Matsuo T, Satterwhite Y, Barrentine SW. Kinematic and kinetic comparison between baseball pitching and football passing. J Appl Biomech. 1996;12:207-224
10. Fleisig, G, Nicholls, R, Elliott, B, and Escamilla, R. Kinematics used by world class tennis players to produce high-velocity serves. Sports Biomech 2: 51–64, 2003.
11. Fleisig GS, Escamilla RF, Barrentine SW. Biomechanics of pitching: mechanism and motion analysis. In: Andrews JR, Wilk KE, editors. , eds. Injuries in Baseball. Philadelphia, PA: Lippincott-Raven; 1998:3-22
12. Gowan ID, Jobe FW, Tibone JE, Perry J, Moynes DR. A comparative electromyographic analysis of the shoulder during pitching: professional versus amateur pitchers. Am J Sports Med. 1987;15(6):586-590
13. Haahr, J. P. “Exercises versus Arthroscopic Decompression in Patients with Subacromial Impingement: A Randomised, Controlled Study in 90 Cases with a One Year Follow up.” Annals of the Rheumatic Diseases 64.5 (2005): 760-64. Web.
14. Ide J, Maede S, Takagi K. Arthroscopic transtendinous repair of partial-thickness articular-side tears of the rotator cuff: Anatomical and clinical study. Am J Sports Med 2005;33:1672-1679.
15. Andrews, James R., Thad S. Broussard, and William G. Carson. “Arthroscopy of the Shoulder in the Management of Partial Tears of the Rotator Cuff: A Preliminary Report.” Arthroscopy: The Journal of Arthroscopic & Related Surgery 1.2 (1985): 117-22. Web.
16. Itoi, Eiji. “Rotator Cuff Tear: Physical Examination and Conservative Treatment.” Journal of Orthopaedic Science 18.2 (2013): 197-204. Web.
17. Jobe CM. Superior glenoid impingement: Expanded spectrum. Arthroscopy 1995;11:530-537.
18. Kibler WB, McMullen J, Uhl TL. Shoulder rehabilitation strategies, guidelines, and practice. Op Tech Sports Med 2000;8:258-267.
19. Jobe, Frank W., and Marilyn Pink. “Classification and Treatment of Shoulder Dysfunction in the Overhead Athlete.” J Orthop Sports Phys Ther Journal of Orthopaedic & Sports Physical Therapy 18.2 (1993): 427-32. Web.
20. Kibler, W. Ben, Aaron Sciascia, and Stephen J. Thomas. “Glenohumeral Internal Rotation Deficit.” Sports Medicine and Arthroscopy Review 20.1 (2012): 34-38. Web.
21. Kronberg M, Nemeth G, Brostrom LA. Muscle activity and coordination in the normal shoulder. An electromyographic study. Clin Orthop Relat Res. 1990;76-85.
22. Kuhn JE, Lindholm SR, Huston LJ, Soslowsky LJ, Blasier RB. Failure of the biceps-superior labral complex: A cadaveric biomechanical investigation comparing the positions of late cocking and early deceleration. Arthroscopy
23. 2003;19:373-379.
24. Kuhn JE, Bey MJ, Huston LJ, Blasier RB, Soslowsky LJ. Ligamentous restraints to external rotation of the humerus in the late-cocking phase of throwing. A cadaveric biomechanical investigation. Am J Sports Med 2000;28:200-205.
25. Liem D, Lichtenberg S, Magosch P, Habermeyer P. Arthroscopic rotator cuff repair in overhead-throwing athletes. Am J Sports Med 2008;36:1317-1322.
26. Lintner, D, Noonan, TJ, and Kibler, WB. Injury patterns and biomechanics of the athlete’s shoulder. Clin Sports Med 27: 527–551, 2008.
27. Manaka, Tomoya, Yoichi Ito, Isshin Matsumoto, Kunio Takaoka, and Hiroaki Nakamura. “Functional Recovery Period after Arthroscopic Rotator Cuff Repair: Is It Predictable Before Surgery?” Clinical Orthopaedics and Related Research® Clin Orthop Relat Res 469.6 (2010): 1660-666. Web.
28. Manske, Robert, Kevin Wilk, George Davies, Todd Ellenbecker, and Mike Reinold. “Glenohumeral Motion Deficits: Friend or Foe?” International Journal of Sports Physical Therapy 8.5 (Oct 2013): 537-53. Print.
29. Matsuo T, Escamilla R, Fleisig GS, Barrentine SW, Andrews JR. Comparison of kinematic and temporal parameters between different pitch velocity groups. J Appl Biomech. 2001;17(1):1-13
30. Mazoue CG, Andrews JR. Repair of full-thickness rotator cuff tears in professional baseball players. Am J Sports Med 2006;34:182-189.
31. Meister K. Injuries to the shoulder in the throwing athlete. Part one: biomechanics/pathophysiology/classification of injury. Am J Sports Med. 2000;28(2):265-275
32. Meister K, Day T, Horodyski M, Kaminski TW, Wasik MP, Tillman S. Rotation motion changes in the glenohumeral joint of the adolescent/Little League baseball player. Am J Sports Med 2005;33:693-698.
33. Nazarian, Levon N. “The Top 10 Reasons Musculoskeletal Sonography Is an Important Complementary or Alternative Technique to MRI : American Journal of Roentgenology: Vol. 190, No. 6 (AJR).” The Top 10 Reasons Musculoskeletal Sonography Is an Important Complementary or Alternative Technique to MRI : American Journal of Roentgenology: Vol. 190, No. 6 (AJR). N.p., June 2008. Web. 20 Feb. 2014.
34. Pappas AM, Zawacki RM, Sullivan TJ. Biomechanics of baseball pitching: a preliminary report. Am J Sports Med. 1985;13(4):216-222
35. Park SS, Loebenberg ML, Rokito AS, Zuckerman JD. The shoulder in baseball pitching: biomechanics and related injuries: part 1. Bull Hosp Jt Dis. 2002;61(1-2):68-79
36. Pradhan RL, Itoi E, Hatakeyama Y, Urayama M, Sato K. Superior labral strain during the throwing motion: A cadaveric study. Am J Sports Med 2001;29:488-492.
37. Proske U, Morgan DL. Muscle damage from eccentric exercise: Mechanism, mechanical signs, adaptation and clinical applications. J Physiol 2001;537:333-345.
38. Reagan KM, Meister K, Horodyski MB, Werner DW, Carruthers C, Wilk K. Humeral retroversion and its relationship to glenohumeral rotation in the shoulder of college baseball players. Am J Sports Med 2002;30:354-360.
39. Reynolds SB, Dugas JR, Cain EL, McMichael CS, Andrews JR. Debridement of small partial-thickness rotator cuff tears in elite overhead athletes. Clin Orthop Relat Res 2008;466:614-621.
40. Riand N, Boulahia A, Walch G. Posterosuperior impingement of the shoulder in the athlete: Results of arthroscopic debridement in 75 patients. Rev Chir Orthop Reparatrice Appar Mot 2002;88:19-27 (in French).
41. Ryu RK, Dunbar WHV, Kuhn JE, et al. Comprehensive evaluation and treatment of the shoulder in the throwing athlete. Arthroscopy 2002;18:70-89.
42. Seldon, Ben. “Is Rotator Cuff Surgery Expensive If I Have Insurance – Most Insurances Accepted.” Is Rotator Cuff Surgery Expensive If I Have Insurance – Most Insurances Accepted. N.p., n.d. Web. 04 Sept. 2016.
43. Seroyer ST, Nho SJ, Bach BR, Bush-Joseph CA, Nicholson GP, Romeo AA. The kinetic chain in overhand pitching: its potential role for performance enhancement and injury prevention. Sports Health. 2010; 2: 135– 146.
44. Shepard MF, Dugas JR, Zeng N, Andrews JR. Differences in the ultimate strength of the biceps anchor and the generation of type II superior labral anterior posterior lesions in a cadaveric model. Am J Sports Med 2004;32: 1197-1201.
45. Stodden DF, Campbell BM, Moyer TM. Comparison of trunk kinematics in trunk training exercises and throwing. J Strength Cond Res. 2008;22(1):112-118
46. Stodden DF, Fleisig GS, McLean SP, Andrews JR. Relationship of biomechanical factors to baseball pitching velocity: within pitcher variation. J Appl Biomech. 2005;21(1):44-56
47. Stodden, David F., Glenn S. Fleisig, Scott P. Mclean, Stephen L. Lyman, and James R. Andrews. “Relationship of Pelvis and Upper Torso Kinematics to Pitched Baseball Velocity.” Journal of Applied Biomechanics 17.2 (2001): 164-72. Web.
48. “Tendon Transfer Procedures.” Shoulderdoc.co.uk. N.p., n.d. Web. 4 Sept. 2016.
49. Thomas SJ, Swanik CB, Higginson JS, et al. A bilateral comparison of posterior capsule thickness and its correlation with glenohumeral range of motion and scapular upward rotation in collegiate baseball
50. Ward, Samuel R., Eric R. Hentzen, Laura H. Smallwood, Robert K. Eastlack, Katherine A. Burns, Donald C. Fithian, Jan Friden, and Richard L. Lieber. “Rotator Cuff Muscle Architecture.” Clinical Orthopaedics and Related Research PAP (2006): n. pag. Web.
51. Walch, Gilles, Aziz Boulahia, Salvatore Calderone, and Andrew H. N. Robinson. “The ‘dropping’ and ‘hornblower’s’ Signs in Evaluation of Rotator-cuff Tears.” The Journal of Bone and Joint Surgery 80.4 (1998): 624-28. Web.
52. Walch G, Boileau P, Noel E, Donell ST. Impingement of the deep surface of the supraspinatus tendon on the posterosuperior glenoid rim: An arthroscopic study. J Shoulder Elbow Surg 1992;1:238-245.
53. Wilk KE, Macrina LC, Fleisig GS, et al. Loss of internal rotation and the correlation to shoulder injuries in professional baseball pitchers. Am J Sports Med 2011;39: 329-335.
54. Walton, Judie, and George A. C. Murrell. “Clinical Tests Diagnostic for Rotator Cuff Tear.” Techniques in Shoulder & Elbow Surgery 13.1 (2012): 17-22. Web.
55. Werner SL, Suri M, Guido JA, Meister K, Jones DG. Relationships between ball velocity and throwing mechanics in collegiate baseball pitchers. J Shoulder Elbow Surg. 2008;17(6):905-908
56. Whitehead NP, Weerakkody NS, Gregory JE, Morgan DL, Proske U. Changes in passive tension of muscle in humans and animals after eccentric exercise. J Physiol 2001;533: 593-604.
57. Wolf, Eugene M., and Vivek Agrawal. “Transdeltoid Palpation (the Rent Test) in the Diagnosis of Rotator Cuff Tears.” Journal of Shoulder and Elbow Surgery 10.5 (2001): 470-73. Web.
58. Ishihara, Yoko, Teruhisa Mihata, Mallika Tamboli, Lauren Nguyen, Kyoung Jin Park, Michelle H. Mcgarry, Shinro Takai, and Thay Q. Lee. “Role of the Superior Shoulder Capsule in Passive Stability of the Glenohumeral Joint.” Journal of Shoulder and Elbow Surgery 23.5 (2014): 642-48. Web.
59. Struyf, Filip, Jo Nijs, Sarah Mottram, Nathalie A. Roussel, Ann M J Cools, and Romain Meeusen. “Clinical Assessment of the Scapula: A Review of the Literature.” British Journal of Sports Medicine 48.11 (2012): 883-90. Web.
