Tensor Fasciae Latae Pain
Symptoms: Tensor fasciae latae pain presents as outer hip pain located at the TFL muscle belly . Pain when lying on the affected side, walking up and downstairs, running, walking, and hiking. Treatable non-surgically within weeks to months with complete recovery probable.
Hi, I’m Sebastian.
This article will share common signs, symptoms, and non-surgical treatments for tensor fasciae latae pain. I’ll also cover some easy home remedies that work very well in the right circumstances!
The 3 home remedies will be exercises shown at the end of the article.
The tensor fasciae latae (TFL muscle) is a hip muscle commonly overactive in many types of athletes. The TFL muscle is part of a group of muscles that tend to become hyperactive, tight, and overused.
Other muscles of the hip region that are also tight in association with tensor fasciae latae tension are the hamstrings, lower spinal erectors, iliopsoas, iliacus (hip flexors), piriformis, and adductor muscles.
Tensor Fasciae Latae Origin and Insertion:The TFL muscle is attached to the IT band at the anterior aspect.. It originates at the pelvis at a location known as the ASIS. It performs various stabilization roles in the pelvis and very little as a primary hip mover.
During a single-leg stance, the tensor fasciae latae function is to stabilize your body in the frontal plane by tensioning the IT band. For this reason, the TFL is called a “fascial tensioner.”
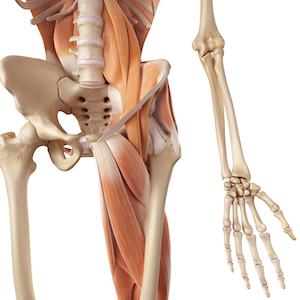
You can see by its small size, it is an accessory muscle in single-leg stance (walking and running), assisting the glute max, hip external rotators, adductors, obliques, and the remainder of the core muscles.
The desire to understand human anatomy, muscles, tendons, and joints is typical in your journey to figure out how to get rid of this problem. Yet, you don’t need to become an expert in human anatomy to eliminate tensor fasciae latae pain.
Understanding what to do and how to do it is vital.
Understanding what is happening in your body is optional.
This article will share some simple solutions that work well for us at Performance Place in Costa Mesa, CA.
Please read this entire article, use the resources/ links I have provided. Recovery could be hiding with a simple exercise or stretch.

Who Gets Tensor Fasciae Latae Pain?
Tensor fasciae latae pain and chronic tightness can happen to anyone at any age. Thought to be a condition of overuse, trigger points tend to occur while performing repetitive activities. Running long distance, HITS training, boot camps, Crossfit METCONs, and even swimming have all been to blame.
Common symptoms first start in the deep gluteal region as a deep ache. It will travel to the front side of the hip and the outer side of the hip. Stiffness in the lower back is commonly associated.
Suppose you are 20-30 years old. In that case, you could be told they have one of the following diagnoses: hip impingement, hip labral tears, hip flexor syndrome, snapping hip syndrome, scar tissue formation, muscle spasms, or early-onset hip degeneration.
If you are over the age of 30, you will more than likely get more diagnoses of degeneration of the hip, osteoarthritis, or trigger points.
As you can tell, the diagnoses are all over the place, which is confusing because you have multiple doctors telling you different diagnoses and different treatment options.
In later sections, we will get into treatments that work exceptionally well for our clients.
Note: Pain, numbness, tingling, or aches that go beyond your knee on the same side is more than likely spine referred.
You do not need to have lower back pain to have spinal referred hip pain.
If you are experiencing these sensations, contact us to help you recover without surgery, medication, or injections.
Tailoring the treatment to your root cause of TFL chronic tightness is essential to get the rapid results you’re looking for.

Causes of TFL Pain
The leading cause of tensor fasciae latae pain is overuse.
Considering WHY it is being overused is where the magic lies.
It’s easy to blame the TFL muscle for working so hard, but if we reverse engineer this process, we will find that the muscular tightness you’re experiencing is nothing more than the squeaky wheel.
Addressing the cause of your tensor fasciae latae trigger point will result in complete recovery. Addressing the squeaky wheel will result in the short-term relief of pain that will not last more than a week in most cases.
Let’s reverse engineer this process.
The TFL muscle is a hip stabilizer. It is NOT a hip mover.
The larger muscles that cross the hip are the prime movers of the hip joint. The muscles that come to mind should be the glute Maximus muscle, the Adductor Magnus, the hamstrings, and the hip flexors/ iliopsoas complex.
90% of the time, the culprit is the inhibition of the glute max muscle (on one or both sides). In the 2000s, this phenomenon was dubbed “glute amnesia.” Clever right?
Why is the glute max so forgetful? Why does it forget to contract?
To reverse engineering this process, we have to ask ourselves how to get maximum glute max contraction.
Maximum glute contraction occurs when the core/ lumbar spine/ pelvis region has adequate stability or reactive stability. Stability is a relative term.
A stable object (let’s say a stack of Jenga block) is only sturdy till the wind blows. Reacting against external forces (wind) to remain upright is the core stability we need to set the stage of reversing glute amnesia.

Consider shooting a cannon from a canoe.
The movement of the canoe as the cannon fires robs the cannonball of distance. Lack of reactive core stability robs you of glute contraction and hip movement. It’s simple physics.
The Mobility, Stability, and Strength Continuum is a simple concept that further explains how the body functions when we reverse engineer tensor fasciae latae pain (as well as other trigger points around the hip).
Simply put, the body is created by a series of alternating mobile and stable joints:
- Midback – mobile
- Low back/ core – stable
- Hip – mobile
- Knee – stable
- Ankle – mobile
- Foot – stable
For this reason, when looking at tensor fasciae latae pain, we may even need to look at thoracic spine mobility to give the core a better ability to keep stable (the canoe).
Here is a Youtube video I made the Mobility, Stability, and Strength Continuum.
Using the Mobility, Stability, and Strength Continuum allows a coach or rehabilitation expert to cleverly design a program to enhance reactive stability where lacking, improve mobility in joints where it has been lost, and then apply strength to the body.
As you can see, it takes more than foam rolling, ART, self-massage, and rest to get rid of tensor fasciae latae pain permanently. While these treatments are great at reducing pain, they do not restore mobility (movement with control), stability, or strength. Weekly treatment should yield long-term results if you ask me!
Where should you start?
While searching the web for the best TFL stretch, may be most people’s instinct, it doesn’t alway yield the best results. A TFL stretch works well for some people, but for many it does not have a lasting effect. If you’re looking for the most effective treatment, having yourself inspected for YOUR reason for TFL spasm is best practice. If you have questions about your specific situation, contact us here.
Yet for you DIYers, I will be showing a few of my favorite exercises for you DIY people using the 5 Step System for tensor fasciae latae pain at Performance Place. Remember, we can coach you virtually if you need help!
Symptoms
Symptoms of tensor fasciae latae pain vary from person to person, based upon their actual diagnosis/ root cause.
Here is a list of what many people experience:
- Worse with running, walking, or jumping
- Less pain with strength training over cardio
- Home HITs training is unbearable
- Feeling like you have to pound your hip
- TFL or IT band spasm
- Adductor muscle trigger points
- Knots in muscles
- Pinchy hips
- Deep glute ache
- Snapping, clicking, or clunking of the hip
- Pressure in the lower back
- Feeling like you need to “pop” your hips or SI joint
You may not be experiencing all of these symptoms, but they are commonly found the longer you have your problem.
Movement compensations tend to create a cascade of associated symptoms that all reversible with the right treatment program and coaching.

Diagnoses
The most common cause of tensor fasciae latae pain in athletes is hip impingement.
- Hip Impingement
- Hip Labral Tears
- Hip Flexor Syndrome (great video on testing impingement vs. hip flexor)
- Sacroiliitis (our Youtube video)
- SI Joint Sprain/ Strain (video)
- Ilioinguinal nerve entrapment
- Lumbar Disc Herniation (video)
- Hip arthritis (careful here, there are many types of arthritis)
- Overuse/ underuse injury
We always have to include the rare but possible sinister diagnoses like a tumor, infection, cord compression, and much more.
To learn more about the “Red flags,” go to this website.

Simple Home Remedies
Reduction of tensor fasciae latae pain comes down to finding out three questions (Part the Performance Place 5 Step System):
1 – A correct diagnosis
2 – What makes you feel better?
3 – What are you doing that keeps the pain around?
Note: If you are interested in how we do things to accomplish rapid success at Performance Place, consider getting access to the Performance Place Hip Program.
1 – A correct diagnosis
Establishing a correct working diagnosis tells us a lot about how to melt your TFL spasm away. The best way to develop a correct working diagnosis is not Google search, WebMD, this article, MRIs, X Rays, or Youtube, believe it or not.
A good old fashion medical history and physical examination by an experienced medical expert is best. A trained eye can identify deficiencies in mobility, stability, and strength that you are not aware of.
Stress testing the hip can be performed, which will rule out many of the diagnoses on the list we had above.
Establishing a “working diagnosis” can happen within 30 minutes. A 5-minute meeting with a doctor or a Youtube video will not accomplish this.
MRIs and X-rays help rule out some diagnoses, but they give very little information about developing and implementing a treatment plan. As you may already know, having a diagnosis and treatment plan does not always improve your situation.
The magic is in HOW you do your exercises, not the exercises themselves. A skilled coach, sports chiropractor, physical therapist, orthopedic doctor, athletic trainer, personal trainer, or medical doctor can help coach these exercises for better results.
Just as professional athletes have skills coaches (a pitching coach in baseball), we all need a little help with our movements to improve.
Lastly, don’t fixate on trying to “see” your problem on an image. Images do not tell us that much information on how to help you.
Images can not see your pain.
Pain is a sensation.
Images can not see thoughts or pain.
Establishing a “working” diagnosis is all you need to start testing the low-hanging fruit in your recovery plan.
2 – What makes you feel better?
Figuring out what makes your TFL feel better or worse can give insight into the mechanics that keep triggering it, which we will cover in the next section.
If laying on your belly feels better, do it more!
If sitting feels better, do it more!
If stretching feels better, again, do it more!
Your body knows what it likes, and you may need to do a little more of it.
3 – What are you doing that keeps the pain around?
Flexion pattern
- Sitting?
- Driving?
- Picking up weights?
- Walking upstairs?
Extension patterns
- Running?
- Walking?
- Walking downstairs?
Specific Activities, Paces, or Durations
- Running?
- Jogging only a particular pace?
- Sprinting a certain distance?
While this may not be an exact science, noting what keeps your TFL in a spasmatic state is worth writing down. It may be worth scaling back on this activity for a week to “reset” your body.
While it’s not what you want to hear, it may be the simplest thing you have ever done. Many of the exercises that help build mobility, stability, and strength needed to reverse engineer this problem may not stick if you keep pissing the area off chronically.
Cooling the TFL down for a week makes it so much easier to coach exercises that help build mobility, stability, and strength.
It’s like working on breathwork while you have a cold; let the body chill out for a week and then proceed. It will make your life way easier!

Non-Surgical Treatment
In my opinion, the best non-surgical treatment for a tight TFL are tensor fasciae latae exercises, or as we call them “active care.”. Active care often needs to be progressed to get you back to the activity you want to do.
Progressive exercises can be tailored to help build support for the motions that trigger your TFL. Think of these exercises as building blocks till you get to the actual activity.
I know all of the “experts,” and your instructor may tell you something else, but hear me out. I’ve been helping runners and lifters with tensor fasciae latae pain in record time for over 12 years now.
I assure you that progressive exercises to build mobility, stability, and strength within regions of the body are the best plan of attack. Custom programming is the best route to go. Proper form can be coached virtual or in person.
Other non-surgical treatments:
Cortisone, Active Release, Rolfing, Adjustments, Prolotherapy, Deep tissue massage; I have tried all of these with many of my dancers with hip pain. None of these treatments work better long-term as a customized mobility, stability, and strength program with good coaching.
Cortisone, Active Release, Rolfing, Chiropractic Adjustments, Prolotherapy, stretching your hip flexor, stretching your hamstrings, and Deep tissue massage are great at reducing pain, but they will not keep it away.
As mentioned before, we need to reverse engineer how you got this way. It did not happen in a day, and it won’t return to normal function in a day either!
Performing the correct exercises and stretches over weeks to months will give you the pain-free hip range of motion that you’ve been looking for.
Challenging corrective exercise is the most effective way.
Corrective exercise can also be a very effective way of reducing pain as well. Allow me to prove it to you.
Here are three simple exercises that you can do as home remedies for chronic TFL and IT band ache.
As a disclaimer, these should not be felt in the TFL at any point. They should feel effortful and painless. Also, know that these DO NOT WORK for everyone. As I mentioned before, your TFL could be in a pissed-off state and not be ready for this type of exercise yet. Here are the best tensor fasciae latae exercises we have found at Performance Place.
Corrective exercises are like medication. If you do the right one in the right situation, you will be amazed at how good it works; you have to keep that feeling with weeks to months of doing the right program.
Note: Some videos may not be live on our Youtube Channel yet. If the video is not live, subscribe and get it when it does.

Recap
If you’re serious about getting over your tensor fasciae latae pain, consider having someone help you. The key is having some with expertise help programming and coach you on what to do.
I wish I could vouch for the skill level of every healthcare provider, physical therapist, chiropractor, acupuncturist, orthopedic, and physiotherapist, but I can’t. We all have different strengths and weaknesses. Myself included.
Off the top of my head, I can estimate that over 90% of clients we have seen with a TFL issue at Performance Place do not need surgery, medications, or injections to return to sport pain-free.
Don’t get talked into doing surgery too soon. You can recover! The human body is remarkably resilient, and it can recover full function on its own with most conditions.
I’m Sebastian at Performance Place Sports Care. We can help virtually or in person. We are in Costa Mesa CA. Rather than tell you how great we are, allow our Google Reviews to speak for themselves.
Our clients have some amazing stories of recovery. Start your recovery story with our help.
Book your first session with us today!
Sebastian
Performance Place®
Virtual & Costa Mesa, CA

